Duration of Treatment
5 to 7 hours of Surgery
Days of Stay
2 months
Anesthesia
General Anesthesia
Cost
80,000 to 10,0000 USD.
LVAD Surgery Cost in India
Understanding LVAD Surgery
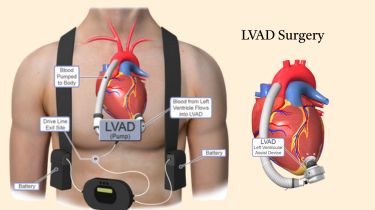
A Left Ventricular Assist Device (LVAD) is a mechanical pump that supports heart function in patients with advanced heart failure. It helps maintain proper blood flow throughout the body when the heart’s ability to pump has declined. This device is often used as a life-saving option for patients awaiting a heart transplant or for those not eligible for transplant.
Estimated Cost of LVAD Surgery in India
India offers LVAD surgery at a significantly lower cost compared to many Western countries, without compromising on quality or success rates. On average:
- Surgery Cost: Between 80,000 to 100,000 USD
- Stay Duration: Around 2 months (hospital and recovery)
- Surgery Time: Typically lasts 5 to 7 hours under general anesthesia
Other Living Expenses:
- Hotel Accommodation (near hospital): 18 to 50 USD per night (varies by service level)
- Food: 20 to 30 USD per day (per person)
- Other daily expenses: Around 20 USD
Final costs can vary depending on the patient’s condition, city, hospital chosen, and type of device used.
Leading Surgeons for LVAD Surgery in India
India is home to some of the most experienced cardiac surgeons with global recognition. Some of the top names include:
- Dr. Naresh Trehan
- Dr. Y K Mishra
- Dr. Z S Meharwal
- Dr. Ramji Mehrotra
- Dr. Kumud Rai
- Dr. Amit Kumar Chaurasia
- Dr. Mukesh Goel
- Dr. Devi Shetty
- Dr. Sandeep Attawar
- Dr. Dhaval Naik
These experts operate in top cardiac centers with advanced infrastructure.
Renowned Hospitals Offering LVAD Surgery
The following hospitals are known for their cardiac care excellence:
- Medanta – The Medicity
- Fortis Heart Institute
- BLK-Max Super Specialty Hospital
- Artemis Hospital
- Manipal Hospitals
- Apollo Hospitals
- Narayana Health
- Saifee Hospital
- Global Hospital
- Yashoda Hospital
- Jaypee Hospital
Each of these centers offers high standards of medical care and patient safety.
Types of LVAD Devices Used in India
Two commonly used LVAD systems are:
- HeartMate 3 – A compact circular pump placed in the heart’s lower chamber. Operated via an external controller using batteries or wall power.
- HeartMate 2 – Slightly older model placed near the abdomen, with similar power connections.
Both devices are used depending on patient need, surgical assessment, and long-term management plans.
Why Choose India for LVAD Surgery?
- Advanced cardiac technology
- World-class surgeons and care teams
- High success rates and global safety standards
- Affordable treatment compared to Europe and the U.S.
- Transparent treatment process with guided support
Symptoms
What Symptoms Might an LVAD Patient Experience?
Patients living with a Left Ventricular Assist Device (LVAD) may experience a range of symptoms related to their underlying heart condition, the presence of the mechanical device, or potential complications. These symptoms are often grouped into categories for easier understanding and management.
- Common and Expected Symptoms
These are typical for individuals with an LVAD and usually do not indicate serious problems:
- Absence of a detectable pulse: Most LVADs produce a continuous blood flow, which can result in a faint or unmeasurable pulse.
- Low blood pressure readings: Patients often have a mean arterial pressure (MAP) between 60–90 mmHg.
- Fatigue: Tiredness is common as the body adjusts to the device and ongoing heart failure.
- Dizziness or light-headedness: This may occur due to changes in blood pressure or volume.
- Warning Signs That Require Medical Attention
Some symptoms may suggest complications and should not be ignored:
- Signs of infection: Redness, swelling, warmth, or drainage at the driveline site, or symptoms like fever and chills.
- Bleeding issues: May occur due to blood thinners. Watch for dark or bloody stools, vomiting blood, or signs of anemia.
- Possible stroke symptoms: Sudden confusion, trouble speaking, weakness on one side—these could be signs of a blood clot.
- Device malfunction indicators: If the LVAD alarms go off, or if you notice fatigue, breathlessness, or dizziness, it might signal a pump issue.
- Heart failure symptoms returning: Swelling in the legs or abdomen, shortness of breath, or increasing fatigue might mean the right side of the heart is struggling.
- Irregular heartbeats (arrhythmias): These may cause fainting, palpitations, or dizziness.
- Low flow alarms: These can result from dehydration, internal bleeding, or pump obstruction.
- Emergency Symptoms – Seek Immediate Help
Some symptoms are considered urgent and require emergency care:
- Severe chest pain or breathlessness: Could indicate pump failure, a blood clot in the lung, or a heart attack.
- Loss of consciousness: May be due to a stroke, device failure, or low blood pressure.
- Heavy bleeding: Especially from the digestive tract or brain.
- Psychological and Emotional Impact
Living with an LVAD can affect mental and emotional health:
- Anxiety or depression: Common due to the lifestyle changes and constant awareness of the device.
- Sleep disturbances: The sound of the pump or emotional stress may disrupt rest.
- Device-Related Sensations
Some experiences may be directly related to the equipment:
- Mild driveline irritation: Slight discomfort near the device cable is common but should not be painful or inflamed.
- Noise or vibrations from the device: This may indicate mechanical issues and should be evaluated promptly.
Monitoring and Ongoing Care
To stay healthy, LVAD patients need regular monitoring and follow-up care:
- Tracking device performance: Speed, power, and blood flow are checked frequently.
- Monitoring blood thinners: INR and other levels are measured to reduce bleeding or clotting risks.
- Watching for signs of trouble: Early detection helps prevent serious complications.
What Are the Key Risk Factors?
Undergoing Left Ventricular Assist Device (LVAD) surgery involves several potential risks, stemming from the procedure itself, the device, and the patient’s overall health. Below is a detailed overview of the primary concerns and contributing factors:
- Surgical Complications
- Excessive Bleeding: Due to major blood vessel handling and the use of blood thinners, bleeding can occur, sometimes requiring transfusion or repeat surgery.
- Infections: Most common around the driveline (where the cable exits the body), infections may spread and cause sepsis.
- Reaction to Anesthesia: Individuals with existing medical conditions may have complications with anesthesia.
- Risks Related to the LVAD Device
- Clot Formation Inside the Pump: Blood clots can develop within the device, potentially causing a blockage or embolism.
- Device Issues: Though rare, hardware problems can lead to reduced function or emergency replacement.
- Driveline Issues: Damage to the cable or infection at the site can lead to complications.
- Unstable Blood Flow: The pump may push too little or too much blood, affecting organ function.
- Cardiovascular-Related Risks
- Stroke: Clots or internal bleeding may lead to brain injury due to anticoagulants and altered circulation.
- Irregular Heartbeats: Abnormal rhythms can strain the heart or lead to collapse.
- Right-Side Heart Failure: As the left side improves, the right side may not cope with increased return flow.
- Blood Pressure Instability: High or low blood pressure can arise based on how the pump is set or individual response.
- Blood-Related Complications
- Increased Bleeding Tendency: Long-term use of blood thinners may trigger internal bleeding, especially in the stomach or brain.
- Clotting Disorders: Continuous blood flow might impair normal clotting mechanisms.
- Red Blood Cell Damage: The mechanical action of the pump can destroy red cells.
- Breathing Problems
- Respiratory Issues: After the procedure, some may develop pneumonia, fluid buildup in lungs, or need extended ventilator support.
- Additional Concerns
- Organ Stress: The liver or kidneys may suffer due to low blood output or surgical strain.
- Mental Health Impact: Anxiety and depression may occur as patients adjust to life with the device.
- Lifestyle Limitations: Managing the external components like batteries and controller can affect daily activities.
Who Is at Greater Risk?
Certain patients are more likely to face complications:
- Seniors or frail individuals
- Those with poor nutritional status
- People with chronic kidney disease, diabetes, or lung pressure problems
- Individuals with previous strokes or bleeding tendencies
- Bedridden or mobility-limited patients
- Anyone with active infections
How to Minimize Risks
- A thorough medical check before the procedure helps reduce dangers.
- Staying under the care of an experienced cardiac team improves outcomes.
- Consistent follow-up helps monitor blood thinning levels, device status, and overall health.
Conclusion
While LVAD surgery can extend and improve the lives of those with severe heart failure, understanding the risks and managing them with a specialized care plan is critical for long-term success.
Preparation for LVAD Surgery
Getting ready for Left Ventricular Assist Device (LVAD) surgery involves careful planning, detailed medical evaluations, and choosing the right care provider. Here’s what patients can expect during the preparation phase:
- Choosing the Right Medical Facility
Start by selecting a reputable hospital in India that specializes in advanced cardiac procedures like LVAD implantation. Cost, surgeon experience, and hospital infrastructure play a major role in successful outcomes.
- Preoperative Medical Evaluation
Before the surgery, a complete set of tests is required to assess heart function and overall health. This includes:
- Blood tests
- Electrocardiogram (ECG)
- Echocardiography (ECHO)
- Urine tests
These tests help determine if the patient is medically fit for the procedure.
- Informed Consent
The patient or family must sign a formal consent document authorizing the medical team to perform the surgery.
- Medication Review
Inform the healthcare team about any current medications, including over-the-counter drugs or supplements. Blood thinners, in particular, are usually stopped at least 7 to 10 days before surgery to reduce the risk of excessive bleeding.
- Hospital Admission
Admission typically occurs a day or two before the operation. Patients are usually asked to fast—avoiding food and drink for several hours before surgery.
- Post-Angioplasty Monitoring (If Applicable)
If the patient has undergone a recent angioplasty, they may need to remain under observation in the hospital for at least one night.
- Understanding the Cost
The cost of LVAD surgery in India can range from approximately USD 80,000 to USD 100,000. This variation depends on factors like the hospital’s location, surgeon’s expertise, and the type of device used.
Procedure
LVAD Implant Procedure
Before undergoing Left Ventricular Assist Device (LVAD) implantation, patients are thoroughly counseled by the surgical and anesthesia teams regarding the expected benefits and potential risks. The procedure is complex and typically requires open-heart surgery under general anesthesia.
Step 1 – Administering Anesthesia
The surgery begins with the administration of general anesthesia to ensure the patient remains unconscious and pain-free throughout the operation. LVAD implantation generally takes between 5 to 7 hours.
Step 2 – Making the Incision
To access the heart, the surgeon makes a vertical incision along the chest. The breastbone (sternum) is then carefully opened to expose the heart.
- The patient is connected to a heart-lung bypass machine, which maintains circulation and oxygen supply during the procedure.
- A ventilator is used to manage the patient’s breathing while the surgery is underway.
- Because the operation is major and tailored to each individual’s condition, recovery time and hospital stay vary from patient to patient.
Step 3 – Implanting the Device
The LVAD is surgically connected to the left ventricle and the aorta. The pump is placed inside the chest, and a driveline (a cable that connects the device to an external power source) is guided through the abdominal wall.
Step 4 – Closing the Incision
After securing the LVAD in place, the surgeon closes the chest using medical sutures, surgical staples, or skin adhesives. The skin is then sealed, and the patient is moved to a specialized cardiac care unit for recovery and monitoring.
post-procedure
LVAD Surgery Post-Care: A Comprehensive Guide
Proper care after a Left Ventricular Assist Device (LVAD) surgery is essential to support recovery, reduce risks, and ensure the device continues to function effectively. Here’s a detailed overview of the post-operative care required for LVAD patients:
- Hospital Recovery Phase
Intensive Monitoring:
After surgery, patients are closely monitored in the ICU. Medical teams track heart function, LVAD performance, and vital signs. In some cases, breathing support with a ventilator is used temporarily.
Pain Control:
Pain is managed through medications to ensure patient comfort.
Fluid Balance:
Electrolyte levels and fluid intake are monitored to avoid complications such as dehydration or fluid overload.
Blood Thinning Medication:
Anticoagulants like heparin or warfarin are administered to prevent blood clots in the device. Regular blood tests help maintain safe dosage levels.
Wound Management:
The surgical site and the driveline exit area are carefully cleaned and dressed to prevent infections.
Gradual Movement:
Physical therapy begins early to improve circulation, strengthen muscles, and support lung function.
- Transition to Home Care
Training for Patients and Families:
- Patients and caregivers learn how to handle the LVAD equipment, including managing alarms and replacing power sources.
- Instructions are provided for driveline care and infection prevention.
- Education on medication adherence and recognizing warning signs like bleeding or clotting is critical.
- Emergency readiness includes carrying identification, knowing when to seek help, and understanding how to respond to emergencies.
Regular Check-Ups:
Patients must attend routine appointments for device assessments, blood tests, and overall health monitoring.
- Lifestyle Modifications
Healthy Eating:
A diet low in salt and rich in nutrients supports healing and helps control blood pressure. Hydration must be balanced to maintain proper flow levels in the device.
Exercise and Activity:
Physical activity should resume gradually. High-impact or risky movements that might affect the driveline must be avoided.
Infection Control:
Strict hygiene practices are important. Patients should avoid exposure to sick individuals or unhygienic environments.
- Emotional and Mental Well-Being
Psychological Support:
Adjusting to life with an LVAD can be challenging. Counseling and support groups help address anxiety, depression, and emotional stress.
Daily Life Adjustments:
Patients must adapt to living with the LVAD’s external components, such as the controller and battery packs, which are worn outside the body.
- Long-Term Monitoring
Ongoing Evaluation:
Doctors regularly check for signs of infection, bleeding, or device problems. Blood work helps track the effects of anticoagulant medications.
Device Performance:
Pump settings are routinely evaluated to ensure the LVAD works properly.
Managing Other Health Conditions:
Patients with diabetes, kidney disease, or right-sided heart failure need integrated care plans to manage these issues alongside the LVAD.
Handling Emergencies:
Being able to identify signs of complications like stroke or pump failure is essential for timely medical intervention.
- Emergency Planning
Patients should always have:
- Extra batteries and a backup controller.
- Contact information for their LVAD medical team.
- Written instructions for emergencies, especially during power outages or equipment failure.
- Rehabilitation Programs
Participation in cardiac rehabilitation programs tailored to LVAD patients helps improve strength, stamina, and confidence. These programs are important for long-term health and quality of life.
Conclusion:
Post-operative care after LVAD implantation is a lifelong commitment. It involves medical management, lifestyle changes, education, and emotional support. A coordinated approach involving doctors, nurses, therapists, and caregivers plays a vital role in ensuring the patient’s recovery and long-term well-being.
Success Rate of LVAD Surgery in India
The effectiveness of Left Ventricular Assist Device (LVAD) surgery largely depends on the patient’s health status, the reason for the implant, and the hospital’s experience. The device may be used for different purposes—supporting a failing heart before a transplant, as permanent therapy for those not eligible for transplant, or temporarily until the heart recovers.
Survival Rates
- After 1 Year: Approximately 80% to 85% of patients are alive after one year with modern LVADs.
- After 2 Years: Around 70% to 75% continue to live with successful outcomes.
- After 5 Years: Survival ranges between 50% and 60%, depending on health conditions and the type of device used.
What Influences the Success Rate?
- Reason for Implantation
- Bridge to Transplant: Patients awaiting a heart transplant often experience better results due to limited duration of use.
- Destination Therapy: Long-term use for individuals not suitable for transplant; success depends on managing ongoing risks.
- Bridge to Recovery: In select cases, heart function improves enough for device removal.
- Type of Device
- Newer continuous-flow pumps, such as the HeartMate 3, are linked with better long-term performance, fewer complications, and improved durability compared to older models.
- Health Condition Before Surgery
- Patients in stable condition and those who are younger generally see better recovery.
- Other health issues like diabetes, kidney damage, or right-side heart problems may lower success chances.
- Poor nutrition or infections before surgery also increase surgical risk.
- Hospital Experience
- Hospitals with skilled surgeons and specialized cardiac care teams tend to report higher success rates.
Potential Complications That May Affect Outcomes
- Infections: Especially around the driveline site.
- Bleeding: Often seen in the digestive tract due to the need for blood thinners.
- Stroke: Both types—blocked vessels or bleeding in the brain—can occur.
- Right Heart Weakness: Sometimes develops after the LVAD is in place.
- Device Issues: Rare, but mechanical problems can still happen.
Impact on Quality of Life
- Most patients experience less fatigue, reduced breathlessness, and improved ability to move and function normally.
- LVAD therapy helps many resume regular activities, increasing independence and energy.
Long-Term Outlook
Despite the challenges, advancements in technology and care methods have significantly improved both survival and lifestyle for patients with end-stage heart failure. For many, LVAD provides a vital option when other treatments are no longer effective.
FAQ
Frequently Asked Questions: LVAD Surgery
Questions to Ask Your Surgeon Before LVAD Implantation:
- Are you specialized and certified in cardiac surgery?
- Is this procedure suitable for my heart condition?
- What are the success rates and how long will my recovery take?
- What are the main risks or complications?
- Which treatment path do you recommend and why?
- How much does LVAD surgery typically cost in India?
- When can I resume regular daily activities and light exercise?
- Will I have stitches, staples, or bandages after surgery?
- Will I require follow-up tests or doctor visits?
- Does your facility offer advanced cardiac care and monitoring?
- Is there a dedicated team for after-surgery support?
- How experienced is your ICU team with heart support devices?
- What are your hospital’s survival outcomes for heart procedures?
What is an LVAD?
A Left Ventricular Assist Device is a mechanical pump that helps the heart pump blood when its natural function weakens. It’s implanted in the chest and supports the left side of the heart.
Who Might Need an LVAD?
This device is commonly used for:
- Patients waiting for a heart transplant (temporary support).
- People not eligible for a transplant (permanent support).
- Individuals expected to recover heart function with assistance.
How Does the LVAD Function?
The LVAD helps circulate blood from the heart to the body, replacing the natural pumping action. Many modern devices use a continuous flow system, which means the patient may not have a noticeable pulse.
Before the Surgery
What Tests Are Needed Before Surgery?
Patients undergo several checks:
- Heart imaging like echocardiograms and scans.
- Blood flow assessments using catheter procedures.
- Laboratory tests for kidney, liver, and blood function.
- Mental health and social support evaluations.
How Should I Prepare for Surgery?
- Follow fasting and medication instructions from your doctor.
- Arrange help for your recovery period.
- Pack personal items for your hospital stay.
During the Surgery
How Is the Surgery Performed?
The operation lasts around 4 to 6 hours and is done under general anesthesia. Surgeons place the pump near the heart and attach it to a power cable that exits through the abdomen and connects to a controller.
What Are the Main Risks?
- Bleeding due to blood thinners
- Infections at the device exit site
- Stroke
- Failure of the right side of the heart
- Technical issues with the device
After Surgery
How Long Is the Recovery?
- Hospital stay usually lasts 2 to 4 weeks.
- Full recovery may take 2 to 3 months, including rehabilitation.
Will I Feel Better Right Away?
Most patients feel improved energy within a few days, but full adjustment to the device takes weeks or months.
Living with an LVAD
How Should I Take Care of the Device?
- Keep the driveline exit site clean and dry.
- Change dressings as recommended.
- Charge and maintain batteries daily.
- Be familiar with the controller alerts and how to respond.
Can I Shower or Travel with an LVAD?
- Special equipment is needed to bathe safely.
- Travel is possible with spare batteries and medical documents.
- Inform security personnel about the device during airport checks.
Will I Need Medication?
Yes. Patients take blood thinners to prevent clotting and other medicines for heart health.
Monitoring and Follow-Up
What Are Signs of Possible Complications?
- Redness, swelling, or discharge from the exit site
- Stroke symptoms like confusion or slurred speech
- Internal bleeding (vomiting blood or dark stool)
- Loud alarms from the controller
How Often Will I Need Checkups?
- Visits are frequent at first and become less regular over time.
Daily Life Questions
Will I Have a Pulse with an LVAD?
Most devices provide continuous blood flow, which might eliminate a detectable pulse. Blood pressure is tracked through mean pressure instead.
Can I Be Physically Active?
Yes, light to moderate activity is encouraged. High-impact or contact sports are not advised.
Is Pregnancy Safe with an LVAD?
Pregnancy is not usually recommended due to medication risks and heart strain.
Long-Term Outlook
How Long Can I Live with the Device?
- One-year survival is approximately 80–85%.
- Many patients live 5 years or more with proper management.
Can the Device Be Removed?
If your heart improves significantly, removal might be possible, though this is rare.
Will I Still Need a Heart Transplant?
If the LVAD was placed as a temporary solution, you’ll remain on the transplant waiting list.
Financial and Emergency Information
Is the Procedure Covered by Insurance?
Most health insurance plans and government programs cover the procedure if medically necessary.
What Are the Ongoing Costs?
- Medication
- Routine appointments
- Battery and equipment replacements
How Should I Prepare for Emergencies?
- Always carry extra batteries and a controller.
- Keep an emergency contact card with device details.
- Contact your healthcare team if any device alarms sound.
What If the Power Fails?
The device runs on battery backups. Make sure extra charged batteries are always available.